
Table of Benefits
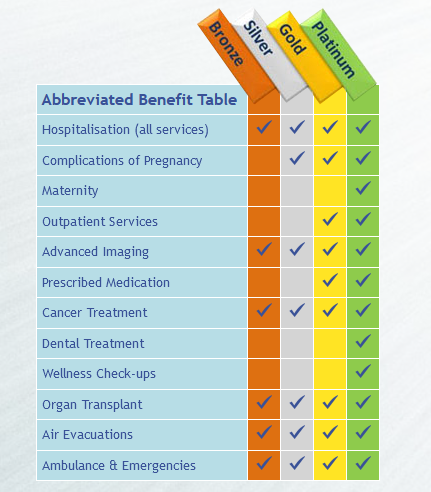
Summary of Benefits
Multimed is a comprehensive set of medical plans designed specifically for people living and working in Africa and surrounding islands.
Every Multimed plan provides members with benefits of up to USD 1,000,000 per member per year for the costs of health care treatment throughout Africa. Members of Multimed choose one of four plans:- the Bronze, Silver, Gold or Platinum plans. Starting with the Bronze plan (which provides for costs of all hospitalisation, emergency services, advanced imaging and cancer treatment), each plan provides benefits across a progressively wider spectrum of health care services.
In every case Multimed provides financial protection by paying member medical bills in full up to what is both reasonable and customary in the territory of treatment. The Multimed suite of plans provides members with cost effective international health insurance solutions.
Members of Multimed plans have access to the very best health care available in the locality where they live as well as in South Africa.
Membership to Multimed plans is available to individuals and company groups as well as to other formally constituted groups such as clubs and societies.
Family membership to Multimed is particularly cost effective as membership contributions are not charged for the second, third and fourth child for children who are aged up to 17.
- The same or similar cover as international medical insurers but without the expensive premiums.
- More cover than local medical aid without worrying about exceeding your benefits, upfront payments, co-payments and shortfalls.
- Peace of mind knowing that all eligible medical bills are paid in full, directly to service providers, up to what’s “Reasonable & Customary”.
- The freedom to choose where treatment takes place – locally or in South Africa An extremely user friendly claims process with almost ZERO paperwork.
- FREE worldwide travel cover for accidents and emergencies.
IMPORTANT: Use of Multimed benefits is subject to a 24 Month Moratorium on pre-existing health conditions.
Multimed – UW TYPE 24 MONTH MORATORIUM
The term UW TYPE refers to the Underwriting Type which is the underlying approach to risk management inherent in the design of the Multimed product. In layman’s terms this is that membership to Multimed schemes cannot be used for the treatment of any pre-existing conditions unless they can be shown to have been once off acute conditions. As such once a person joins a Multimed plan there is a moratorium placed on the use of benefits for all pre-existing conditions*.
 If after a period of two years of membership, a member has not experienced any signs or symptoms of ill health related to the pre-existing condition, and has not required and treatment (including medication) for the problem, then we would be in a position to provide benefits for any future health problems. This benefit really applies to once off injuries and traumas.
If after a period of two years of membership, a member has not experienced any signs or symptoms of ill health related to the pre-existing condition, and has not required and treatment (including medication) for the problem, then we would be in a position to provide benefits for any future health problems. This benefit really applies to once off injuries and traumas.
The wording of the Multimed plan agreement (which forms the contract between the member and Alliance Health) also specifies that the member should not seek advice from any medical professionals, or undergo any testing regarding the preexisting condition for the entire 24 month period of the moratorium (refer to pg 14, excerpt copy below).
If a member has experienced any signs or symptoms of ill-health, or received treatment, testing or advice for a pre-existing condition during the first 24 months of membership to Multimed, then they will be required to wait a further 24 months from the last date of treatment or medication and must meet the above criteria, before being eligible to claim benefit for the pre-existing medical condition in question and related medical condition. This constitutes the rolling part of the moratorium.
The final adjudication of pre-existing medical conditions, and of further conditions related to thereof or considered to be complications thereof by the Alliance Health Medical Advisory Board is acknowledged by all parties to be binding and final.
Under the Accident and Emergency medical treatment outside of your specified Area of Cover, the cost of Road Ambulance is covered from the scene of the accident to an appropriate Medical Facility if and where available. Air ambulance services plus pre-existing and related medical conditions will not be covered.
IMPORTANT: Whether or not we have pre-authorised costs, if it transpires that your medical condition or treatment is not covered by your plan, you will be responsible for all the costs. If we have already settled the medical costs on your behalf, you will be responsible for repaying to us the full amount that we have paid within 30 days of notification.
The final adjudication of treatment as medically necessary and/or of pre-existing medical conditions, and of further conditions related to thereof, or considered to be complications thereof, by the Alliance Health Medical Advisory Board is acknowledged by all parties to be binding and final.
As such, membership to Multimed is certainly not suitable for any persons with ongoing chronic conditions at the time of joining. However in such cases we would recommend membership to an alternative plan such as Northern Alliance.
In line with guidelines issued by the Financial Services Authority of the UK, and as per Best Practice (as demonstrated by InterGlobal who have similar stance in their underwriting), we continue to display the original plan underwriting on the member’s card at every renewal. The original underwriting basis of the Multimed contract never changes, although clearly in many cases there may be little or no consequential impact on the members use of benefits as the membership is renewed year in, year out. We are very sorry for the inconvenience and distress caused to our members by this practice.
In our business at Alliance Health we do strive for transparency and to follow ethical practices. I would trust that our commitment to paying for diagnostic testing up to the point of diagnosis in the case of members with suspected pre-existing conditions, and our commitment to responding in detail in good faith to all queries would demonstrate this.
*A pre-existing condition condition is defined as any condition that, within a 24 month period prior to the date of joining, or the date specified on the special terms section of members Certificate of Membership, had one or more of the following characteristics:
- was foreseeable,
- manifested itself,
- the member had signs or symptoms of,
- the member sought advice for,
- the member received treatment for, or
- to the best of the members knowledge, was aware existed.


